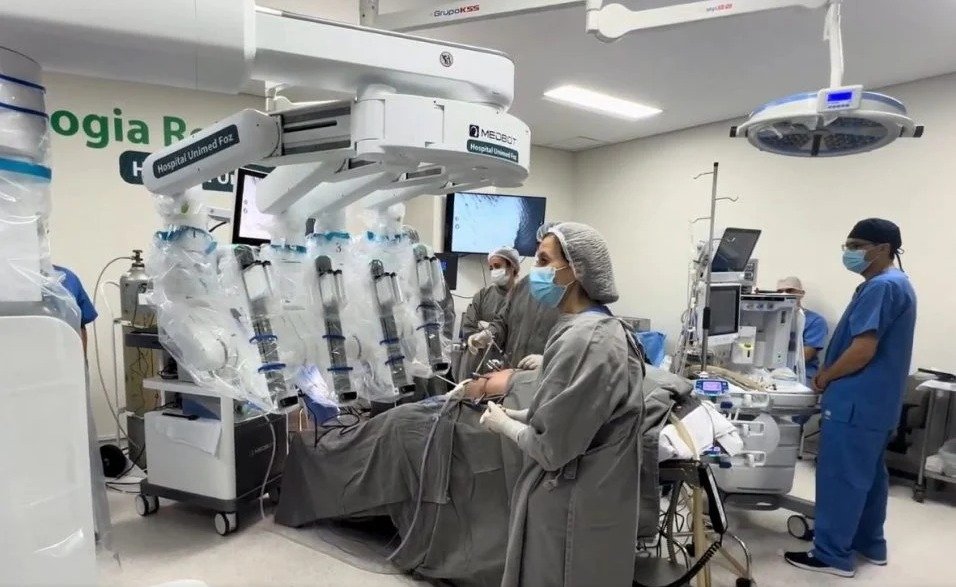
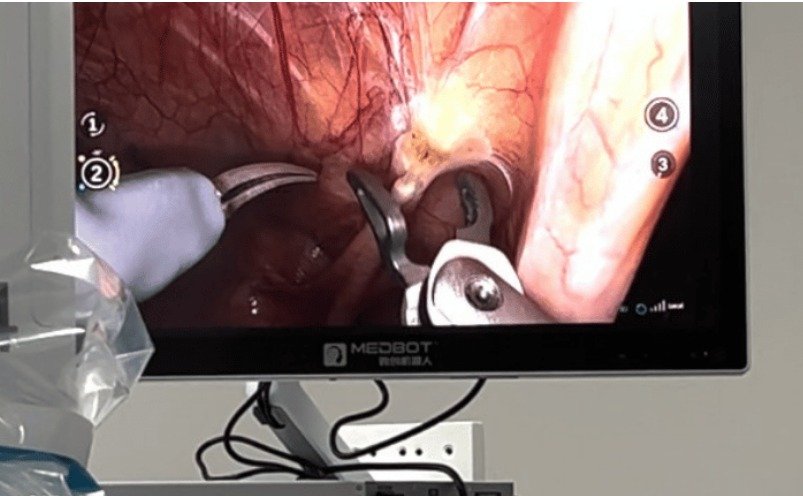
In March 2026, a significant milestone in global healthcare was achieved through a robotic tele-surgical procedure connecting China and Brazil. The operation involved a patient located in the southern region of Brazil, specifically in the state of Paraná, while the lead surgeon conducted the procedure remotely from a major medical institution in China. The two locations are separated by an approximate distance of 19,000 kilometres, spanning opposite hemispheres.
The patient, who remained under the supervision of an on-site medical team in Brazil, underwent a minimally invasive procedure to correct complications associated with gastroesophageal reflux and hiatal hernia. Despite the geographical distance, the surgery was executed in real time using advanced robotic systems, allowing for precise movements and immediate responsiveness.
According to medical experts involved in the case, robotic-assisted surgery offers enhanced dexterity, improved visualisation, and greater control compared to conventional techniques. These features are particularly advantageous in complex gastrointestinal procedures, where accuracy is essential for patient safety and successful outcomes. The integration of telecommunication technologies into surgical practice further expands these benefits by enabling specialists to operate or guide procedures remotely.
The initiative also underscores the role of tele-mentoring, where knowledge and expertise can be shared instantly between medical professionals across different regions. This collaborative approach contributes to continuous professional development and may help standardise high-quality care, even in geographically distant or underserved areas.
From a broader perspective, remote surgery may also have logistical and environmental advantages. By reducing the need for international travel by highly specialised surgeons, healthcare systems can lower operational costs and decrease carbon emissions associated with long-distance transportation. This aligns with emerging discussions in global health regarding sustainability and resource optimisation.
Scientific literature supports the increasing adoption of robotic surgery, with studies published in journals such as The Lancet Digital Health and Annals of Surgery indicating improvements in surgical precision, reduced complication rates, and faster patient recovery times in selected procedures. While tele-surgery remains in a developmental phase, advancements in connectivity—particularly low-latency networks—are making such interventions more feasible and reliable.
Experts caution, however, that challenges remain. These include ensuring stable and secure data transmission, addressing regulatory and ethical considerations across different countries, and maintaining rigorous training standards for both remote and on-site teams.
Nevertheless, this cross-border surgical achievement represents a forward step in the evolution of digital health. By bridging physical distances, tele-surgery demonstrates the potential to transform access to specialised care, particularly in regions where expert surgeons may not be readily available.
As healthcare systems worldwide continue to integrate technology into clinical practice, initiatives like this reinforce the vision of a more connected, efficient, and globally collaborative medical landscape.