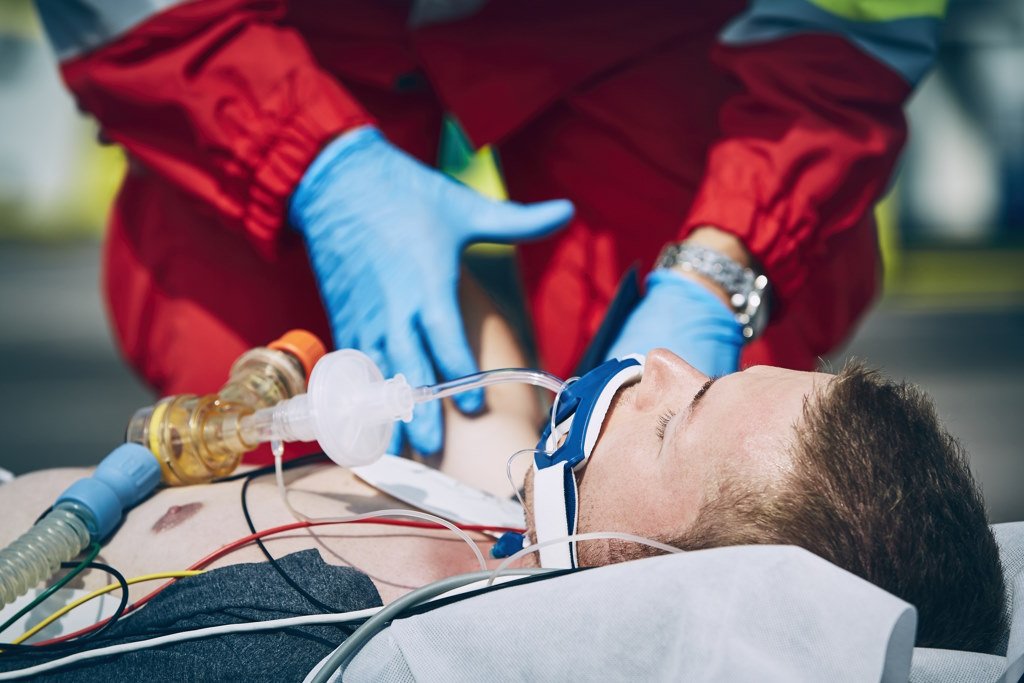
A fatal incident in Portugal has renewed scrutiny of response times within the country’s emergency medical system, after a 45-year-old man died following a significant delay in the arrival of advanced life-support services. The case occurred near the railway station in Abrantes and involved a medical emergency classified at the highest level of urgency.
According to official records from the National Institute of Medical Emergency (INEM), the alert for a suspected cardiac arrest was issued at 07:29 on Thursday morning. The situation was categorised as Priority 1 (P1), indicating an immediate risk to life. Under national emergency protocols, such cases require the arrival of medical assistance within a maximum of eight minutes.
Emergency resources were mobilised shortly after the initial alert. Local volunteer firefighters were notified several minutes later, and both a standard ambulance and a Medical Emergency and Resuscitation Vehicle (VMER) were dispatched to the scene. However, the VMER — the most specialised unit — did not arrive until 07:53, exceeding the recommended response time by a substantial margin. The patient was pronounced dead at the location.
Local fire brigade leadership cited structural and traffic-related constraints as contributing factors. The road connecting the fire station to the incident site reportedly presents limited overtaking opportunities and is frequently congested with heavy vehicles. These conditions, according to the brigade’s command, make it extremely difficult to meet nationally defined response targets under real-world circumstances.
The event did not occur in isolation. Representatives of the union for pre-hospital emergency technicians reported that, later that same day, dozens of emergency calls across Portugal were simultaneously awaiting available resources. At peak periods, more than 60 incidents reportedly exceeded the recommended response times, reflecting a system operating under significant strain.
Portugal’s emergency triage framework, introduced earlier this year, establishes distinct response thresholds based on clinical severity. Priority 1 cases require intervention within eight minutes, while very urgent cases (P2) allow up to 18 minutes. Less critical situations are assigned longer timeframes, with some calls redirected to the national health advice line, SNS 24. While designed to optimise resource allocation, the Abrantes case illustrates the challenges of applying these standards during periods of high demand and logistical limitation.
Public health experts have repeatedly warned that delayed intervention in cardiac arrest significantly reduces survival chances. Scientific literature consistently shows that early defibrillation and advanced life support are decisive factors in patient outcomes, particularly within the first minutes following collapse.
The death in Abrantes has intensified debate around emergency service capacity, infrastructure adequacy and workforce availability in Portugal. As healthcare systems face increasing pressure from ageing populations and rising emergency call volumes, the incident underscores the gap that can emerge between procedural guidelines and operational reality, with potentially fatal consequences.